Why Am I So Tired? The Link Between Blood Sugar, Stress & Life
Why am I so tired?
It’s a big question and truthfully, too big for one blog post. But today I want to focus on one piece of the puzzle that I come back to often:
blood sugar regulation.
This is something I care deeply about both personally and professionally. I’ll share a little of my own journey, in the hope that more people will dive deeper into this earlier than I did.
Looking back, I can see that my blood sugar has been unstable since my teenage years, maybe earlier. By my early twenties, it had become noticeable enough that I always felt like I needed access to food, just in case. Because sometimes if I didn’t eat regularly, I would get nauseated, feel shaky, become short tempered and my brain and eyes would feel ‘funny’.
When I fell pregnant for the first time, I mentioned this to my GP/Obstetrician. I was told it sounded like low blood sugar and not diabetes. And at the time I didn’t ask to investigate it further.
I fainted during my first pregnancy glucose challenge, so it was abandoned. In my second pregnancy, I failed the test (meaning I had gestational diabetes), but the results weren’t reviewed until I was only weeks out from my due date. At that point, everything became a bit of a scramble to manage.
After that pregnancy, I went on to fail another glucose challenge test and this time as I was not pregnant, I was formally diagnosed with Type 2 Diabetes. For my third pregnancy I required insulin and I was checking my blood sugars up to 10 times per day. After my third child, follow up medical advice was that I would probably be on pharmaceutical medication for diabetes by the time I was 40 and just see how I go!
Well, I’m now nearly 9 years past that point and not on any diabetes medication, but it’s something that I work on every day.
Type 2 Diabetes is a condition where the body is no longer effectively able to regulate blood sugar, meaning glucose builds up in the bloodstream rather than being moved into the cells where it’s needed.
It’s incredibly common and often associated with lifestyle factors such as diet, movement, and weight.
But not always.
One of the most important messages behind this blog is that metabolic health doesn’t always look the way we expect it to.
You can’t tell if someone has poor blood sugar regulation just by looking at them.
And this is something I’ve lived.
We hear the word diabetes often, along with numbers like fasting blood sugar and HbA1c. But we don’t talk as much about how it actually feels to live in a body where blood sugar isn’t stable. And let me tell you, it’s not easy!
Blood sugar dysregulation affects more than just numbers on a test. What many people may not realise is that blood sugar fluctuations themselves can directly impact energy metabolism and contribute to both physical and mental exhaustion. Over time, the stress of managing these swings can lead to feelings of failure, burnout, and disengagement from self-care routines, further exacerbating sugar instability and increasing the risk of diabetic complications later in life.
So, when someone asks: ‘Why am I so tired?’
Blood sugar can be one of the contributing factors. And like many health conditions, blood sugar doesn’t exist in isolation and is shaped by:
stress
lifestyle
life seasons
nervous system load
and the capacity you have at the time.
What My Blood Tests Actually Showed Over Time
I always keep copies of my blood tests, and I encourage my clients to do the same.
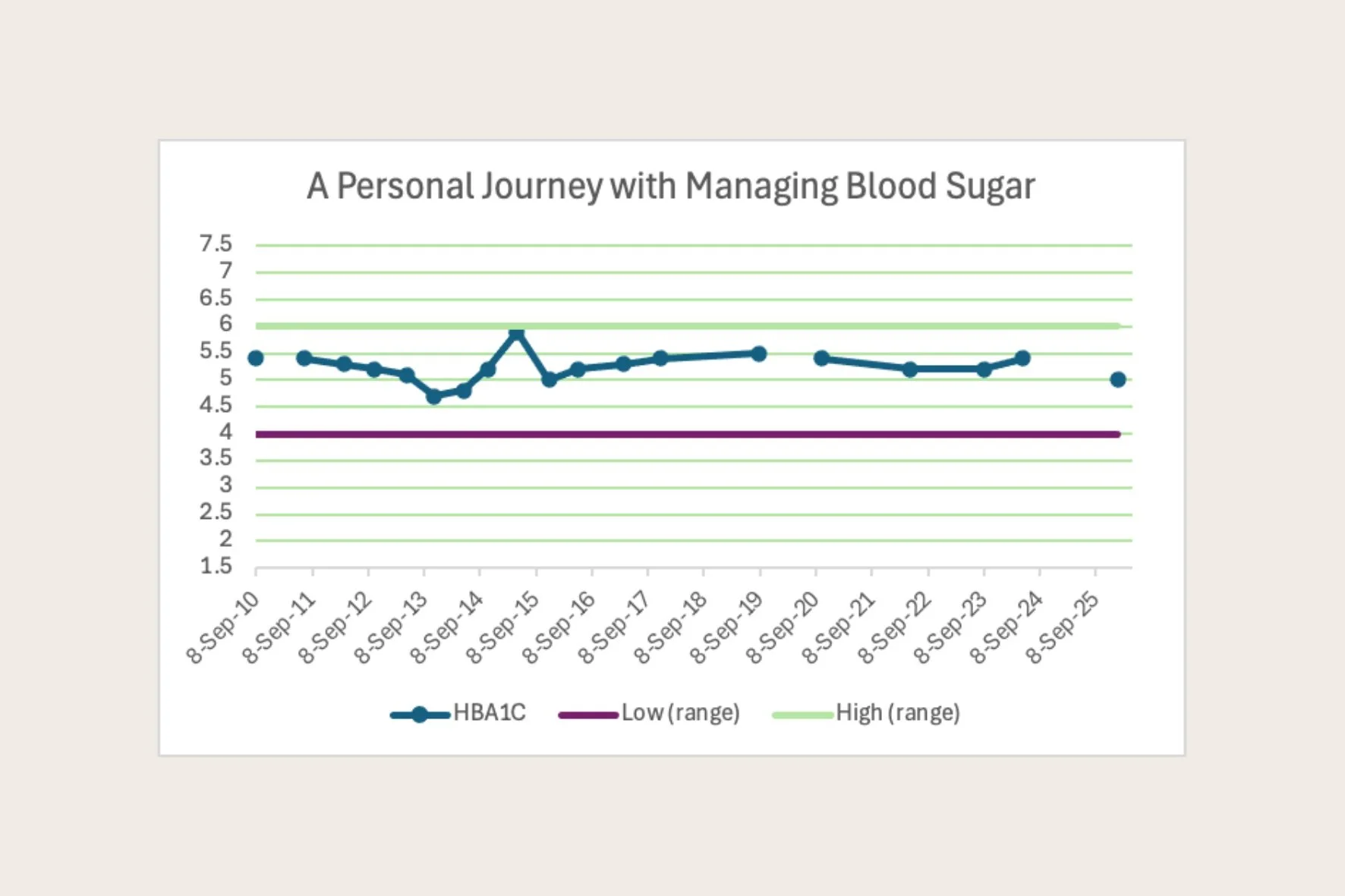
Recently, I went back through my records and graphed my HbA1c over time.
My first recorded result was in September 2010, during the last trimester of my third pregnancy. My most recent result is from January 2026.
Looking at this data has been incredibly personal but also incredibly insightful so I wanted to share just how life impacts blood sugar.
HbA1c is used to assess how well your blood sugars are managed (see below), but what it doesn’t show well is variability, the ups and downs, the swings and the crashes.
And in my experience, those swings between high and low blood sugar readings are what creates many of the symptoms I described above.
HbA1c reflects your average blood glucose over approximately three months, and it’s commonly used to assess long-term blood sugar control.
When I look at my results over time, I can clearly see different phases.
Phase 1: Foundation & Stability
After the birth of my third son in late 2010, my levels stabilised and began to decrease as pregnancy hormones settled. This was a time where my focus was very much on home life, raising children, improving diet, and simplifying things.
There was a strong focus on food and routine.
And you can see that reflected in the numbers.
Phase 2: Lifestyle Drift & Wake-Up Call
Following this there was a period where my lifestyle choices weren’t as supportive and this time correlates with my highest reading of 5.9 (this is right on the upper limit of what is accepted normal).
This was a more social phase of life, with less structure and more variability.
That result was a shock and a turning point. I made significant changes and the very next reading dropped significantly. These changes were entirely lifestyle-driven, I wasn’t using supplements or herbs just making different choices.
A reminder of how responsive the body can be.
Phase 3: High Demand Years
The next phase of my life was demanding, with lots of change.
This included:
university
career transition into naturopathy
separation
building a business
There was a lot of stress, a lot of pressure, and likely elevated cortisol all of which impact blood sugar regulation.
Even without dramatic spikes, you can see a subtle upward shift.
This period of life wasn’t about poor choices, it was about life load.
Phase 4: Recalibration & Healing
More recently, as a practicing naturopath, I’ve explored different ways to support my blood sugar including herbs, supplements, and continuous glucose monitoring.
The downward shift hasn’t come from any one intervention it’s been a combination of everything.
From:
consistent movement
better understanding of my body
more supportive food choices
and creating more balance overall
And as a result, this is where you start to see the numbers come down again, my lowest reading for 10 years!
When I saw this mapped out over time, it stopped being about numbers and started telling a story.
Even when you’re doing healthy things, chronic demand can still dysregulate metabolism and show up in blood sugar readings.
Future goal is to bring my HBA1c back under 5.
What Actually Helped
Nutrition
My degree and ongoing education as a naturopath involves a substantial focus on nutrition and it really is one of the key foundations when it comes to managing blood sugar.
Your food choices absolutely matter. They can be the difference between a productive, steady day and a complete crash.
That said, nutrition is not one-size-fits-all.
What has helped me most is focusing on the basics:
adequate protein with each meal
consistent meal timing
good fats
whole foods and eliminating processed foods
refuelling properly after exercise
Together, these support me throughout the day.
If this sounds like something you’d like to work on click here to make an appointment.
The Role of Stress
One of the pieces of the puzzle, and one that is often underestimated, is stress.
Stress impacts blood sugar in two key ways.
Firstly, there is a direct physiological effect.
When the body is under stress, hormones like cortisol and adrenaline are released. These signal the liver to release glucose into the bloodstream, while also reducing how effectively insulin works.
In simple terms:
stress not only raises blood sugar, it makes it harder to bring it back down.
Secondly, there is an indirect effect.
Stress influences behaviour.
It affects how we eat, how we move, how we sleep, and how consistently we follow through with the things we know support us.
Not because we don’t care but because our capacity is reduced.
Over time, this can contribute to what is often described as ‘diabetes burnout’.
The constant management, the unpredictability, the feeling of not quite getting it right it can become exhausting.
And this, in turn, can further worsen blood sugar control.
So when we talk about managing blood sugar… we have to talk about stress.
Alcohol & glucose
I get asked about alcohol a lot.
And the honest answer is it depends on where you’re at and what your individual goals are.
If you’re trying to regulate blood sugar, improve energy and mood, or support metabolic health, alcohol will make that harder.
Alcohol is known too:
disrupts blood sugar regulation
impacts sleep
places additional load on the liver
alcohol alters intestinal microbiota composition, increasing the permeability of the intestinal lining, leading to intestinal and then widespread inflammation.
For some people, reducing alcohol is one of the most impactful changes they can make.
Continual Glucose Monitor insight
Last year I decided to try a continuous glucose monitor (CGM). This a small device that you attach to your arm for two weeks so you can see exactly what your blood sugar readings are at all times.
I had been putting it off for a long time.
Partly because I knew my levels were sensitive I was worried about how bad the results would be. And it also brought back memories of pregnancy and being told my sugars had to be ‘perfect’ and the constant stress of managing that time of my life.
So, there was a lot tied up in it.
But when I finally did it, it was a relief as I have learnt and gained important information that supports me to make better decisions and feel better too.
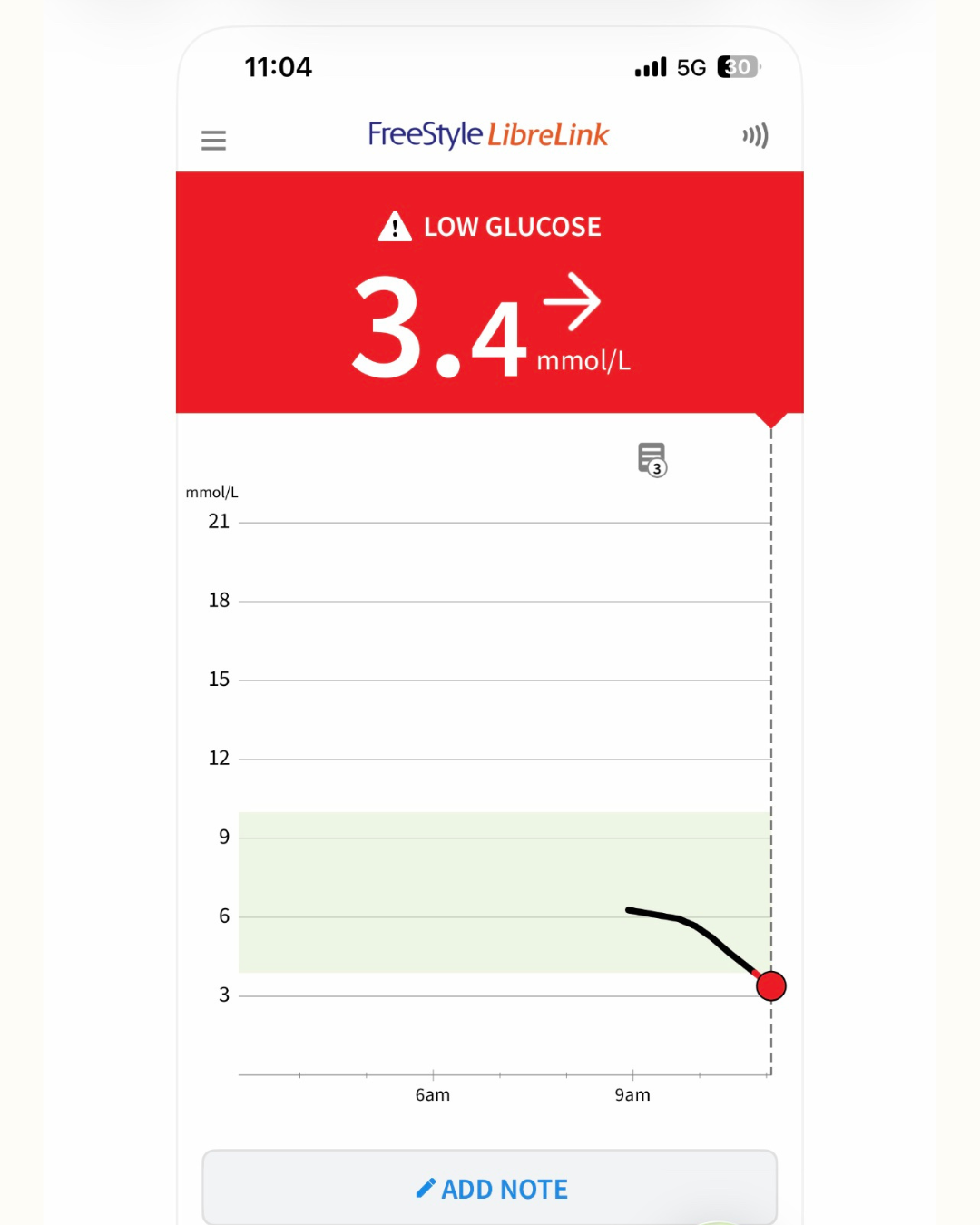
Screen shot from the CGM app showing my levels below recommended blood sugar levels. I felt symptoms of low blood sugar and needed to eat something straight away.
And yes I saw it all:
lows around 3.4
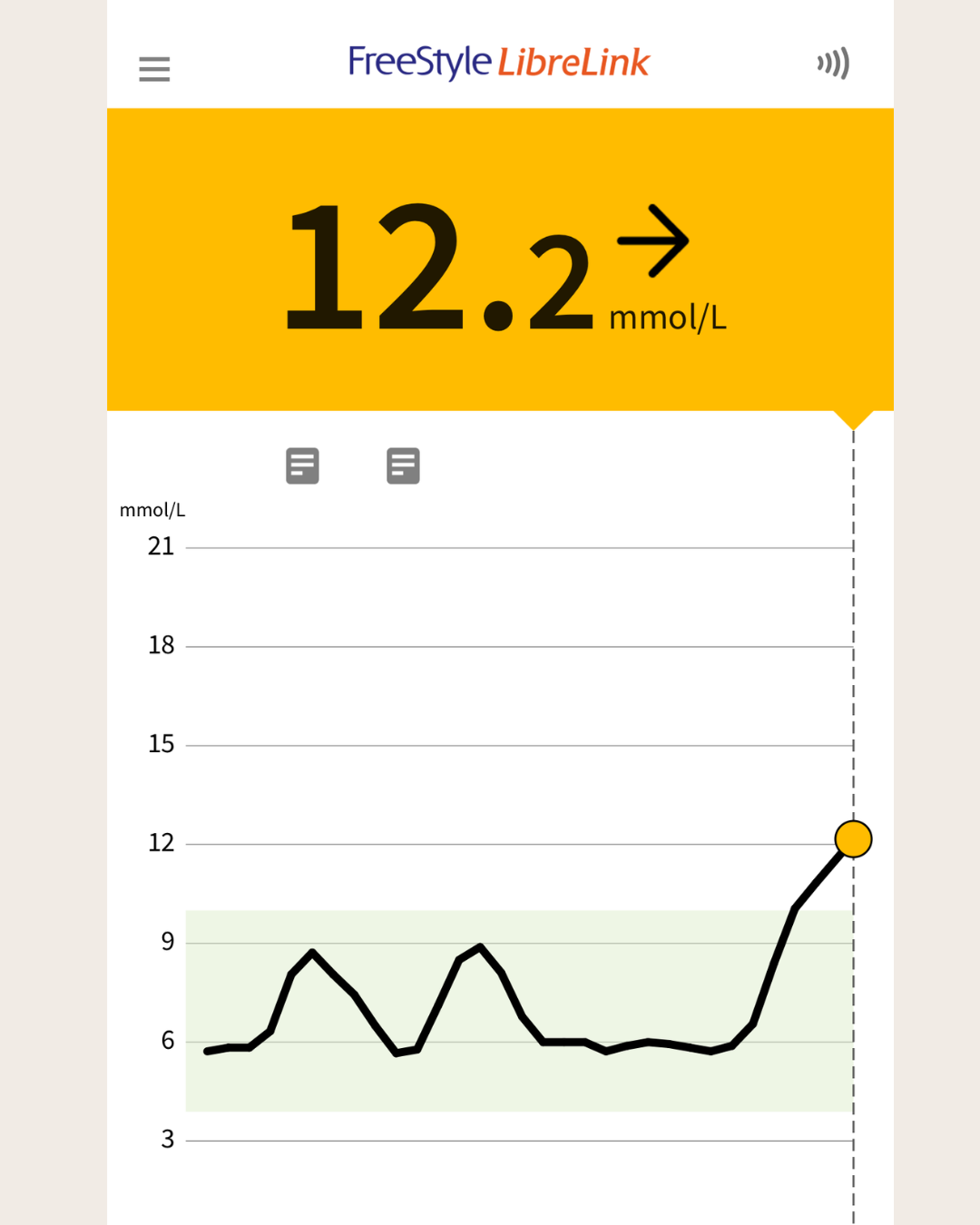
highs above 12
But more importantly, it gave me clarity.
Screen shot from the CGM app showing my levels above recommended blood sugar levels.
For years, I had experienced:
needing to eat frequently
feeling shaky or unwell if I didn’t
energy crashes
racing heart rate rate (this happens to me when my sugars are too high)
generally, not feeling well and wondering if it was my sugars again!
With the CGM I could instantly see what was happening which not only helped me learn what foods I definitely should not be eating, but also reinforced the link between how I felt in my body and my blood sugar readings. This was incredible information and allowed me to make a lot of changes confidently!
I have known since I started checking my sugars that my results swing high and low, I understand now that this is a classic picture of reactive hypoglycemia.
Reactive hypoglycemia is where blood sugar rises and then drops quite quickly after eating, often within a few hours and leads to these very real symptoms.
It’s not always picked up in standard testing, and it doesn’t always fit neatly into a diagnosis early on.
But when you see it both in symptoms and in real-time data it makes a lot of things make sense.
Consistency Over Perfection
When making lifestyle and diet changes, what has mattered most is not doing everything perfectly but doing the basics consistently.
focusing on protein
moving regularly
supporting your nervous system daily, even in small ways.
The body takes time to adjust and learn that there is a new way, keep going.
Reframing Diabetes & Metabolic Health
Without a doubt, some of the most complex cases I see in clinic involve metabolic health.
It is not something you can assess purely based on body shape or size, a diet recall or even a single blood test.
Because blood sugar doesn’t exist in isolation.
It responds to:
diet choices
nutritional deficiencies
stress
sleep
nervous system load
daily demands
and the capacity you have at the time.
There have been periods in my own life where, on paper, I was doing a lot of the ‘right’ things…
But my body was still under pressure.
And that showed up in my blood sugar.
Key points to consider:
how supported the nervous system is
how much stress the body is under
diet
and whether what we’re asking of the body is actually sustainable
Because when the body is constantly trying to keep up…
Something will shift.
And often, blood sugar is one of the first places we see it.
All of this can sound complex and in many ways, it is.
But that doesn’t mean you need to do everything at once.
A good place to start is with the basics:
eating regularly and including enough protein
getting consistent movement
and beginning to support your nervous system in small, realistic ways
Not perfectly, just consistently.
Closing
What I would encourage is this:
If you’re tired, if your energy feels unstable, or if your body isn’t responding the way it used to…
it’s worth looking deeper and looking at things holistically.
And don’t discount blood sugar as a factor just because your HbA1c and fasting glucose are within range.
Blood sugar dysregulation is real, and the symptoms can have a significant impact on your day-to-day quality of life.
Maybe my story is less common now, with more awareness around metabolic health.
But many people are still being missed especially those who don’t fit the ‘expected picture’.
If you’d like a simple starting point, I’ve created a handout:
Daily Goals for Better Metabolic Health
You’re welcome to message me via @kingfishernaturopathy or email me at susan@kingfishernaturopathy.com.au and I’ll send it through.
And if you’re ready for more personalised support, you can book a consultation here.
References
Lorenzo, J. (2026). Nutritional Approach to Alleviate Fatigue in T2DM, a Narrative Review. EC Nutrition,
Saraei, F. H., Hatami, H., & Bagheri, F. (2016). Effectiveness of stress management on glycemic control and change of some of mental health indicators (depression, anxiety, stress, and quality of life) among patients with type 2 diabetes. Mediterranean Journal of Social Sciences, 7(4).
Suresh, K. (2024). Reactive Hypoglycaemia-A challenge for Diabetes Management!. Blood, 1, 2.21, 01-15.
Wu, T. E., Su, Y. W., & Chen, H. S. (2022). Mean HbA1c and HbA1c variability are associated with differing diabetes-related complications in patients with type 2 diabetes mellitus. Diabetes research and clinical practice, 192, 110069.